Forskning på NIV i hjemmet for KOLS

Les om viktige funn fra nyere klinisk forskning og betydning for behandlingsbeslutninger og pasientutvelgelse.
Hva er de evidensbaserte fordelene med NIV i hjemmet for KOLS?
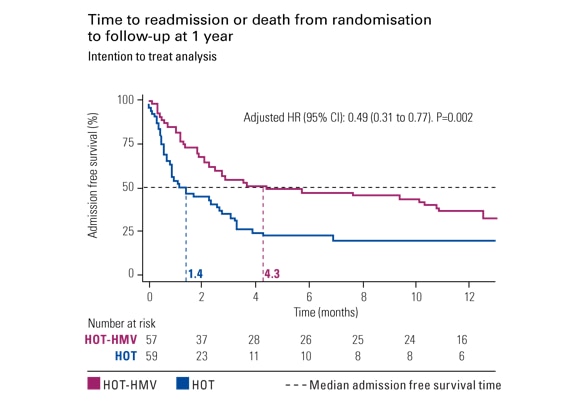
HOT-HMV-studien
HOT-HMV-studien1har vist en 51 % reduksjon i risiko for reinnleggelse på sykehus eller dødsfall hos hyperkapniske KOLS-pasienter behandlet med ikke-invasiv ventilasjon og oksygenbehandling i hjemmet.
Kostnadseffektivitet for HOT-HMV-behandling
Etter utfallet av HOT-HMV-studien1 ble det utfør en helseøkonomisk analyse for å vurdere kostnadseffektiviteten av HOT-HMV sammenlignet med HOT alene blant KOLS-pasienter i Storbritannia med vedvarende hyperkapni etter en livstruende eksaserbasjon.2
Analysen antyder at sannsynligheten for at HOT-HMV er kostnadseffektiv, er 62 %, basert på villighet til å betale 30 000 pund.
Köhnlein-studien
Reduksjon i dødelighetsrisiko med 76 % over 1 år med NIV3
Denne randomiserte, kontrollerte studien viste en vesentlig forbedring i overlevelse for stabile hyperkapniske KOLS-pasienter som ble effektivt behandlet med NIV.
Forbedret livskvalitet3
Ved hjelp av St Georges respirasjonsspørreskjema viste studien også at pasienter behandlet med NIV rapporterte en vesentlig forbedret livskvalitet
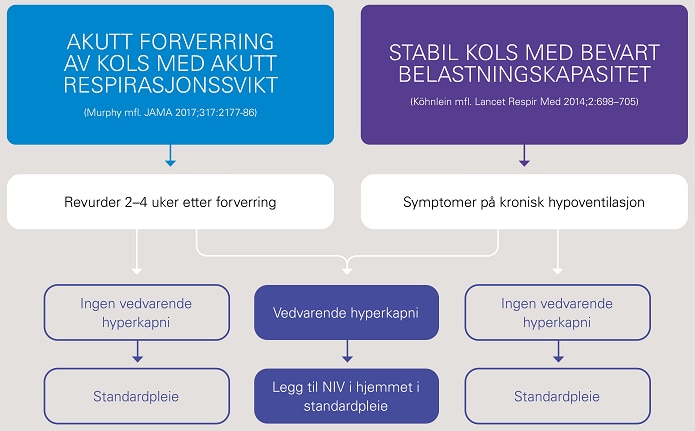
Flytdiagram som viser pasientutvelgelse for NIV i hjemmet basert på kliniske studiedata.1,3
GOLD-retningslinjer
Retningslinjene fra Global Initiative for Chronic Obstructive Lung Disease (GOLD) angir at NIV i hjemmet kan forbedre sykehusinnleggelsesfri overlevelse hos utvalgte pasienter etter nylig sykehusinnleggelse, særlig pasienter med markert vedvarende hyperkapni om dagen (PaCO2 ≥ 52 mmHg’, evidensnivå = B).5
ERS-retningslinjer
En tverrfaglig ERS-arbeidsgruppe har publisert evidensbaserte anbefalinger som betinget støtter bruk av LTH-NIV for å forbedre helseresultater ved hjelp av faste trykkinnstillinger og mål om en reduksjon i karbondioksid hos KOLS-pasienter med vedvarende hyperkapnisk respirasjonssvikt.6
Pasientoppfølging
Oppfølgingen av pasienter kan forenkles med teknologi for telemonitorering som tilbyr ventilasjonsdata, asynkroni mellom pasient og ventilator, transkutane gassmålinger og andre relevante parametere. Omhyggelig oppfølging er vesentlig for pasienter som har startet på høyintens NIV.
[Webinar] NIV i hjemmet ved stabil KOLS: HVORDAN og HVORFOR?

Professor Windisch bruker eksempler fra sin mer enn 20-årige erfaring for å utforske utviklingen av behandlingen fra tidlige negative studier ved hjelp av ventilasjon med lavintensitetstrykk til dagens evidensbaserte metode med NIV for å redusere CO2 maksimalt med riktig pasientutvelgelse for å forbedre overlevelse og livskvalitet hos pasienter med stabil hyperkapnisk KOLS.
Referanser:
*Som vist ved resultater etter 3 og 6 måneder for livskvalitet og etterlevelse
- Murphy P et al. Effect of Home Noninvasive Ventilation With Oxygen Therapy vs Oxygen Therapy Alone on Hospital Readmission or Death After an Acute COPD Exacerbation. A Randomized Clinical Trial, JAMA. Published online May 21, 2017. doi:10.1001/jama.2017.4451.
- Murphy PB et al. Cost-Effectiveness of Home Oxygen Therapy-Home Mechanical Ventilation (HOT-HMV) for the Treatment of Chronic Obstructive Pulmonary Disease (COPD) with Chronic Hypercapnic Respiratory Failure Following an Acute Exacerbation of COPD in the United Kingdom (UK). American Journal of Respiratory and Critical Care Medicine 2018;197:A2517.
- Köhnlein T, et al., Non-invasive positive pressure ventilation for the treatment of severe stable chronic obstructive pulmonary disease: a prospective, multicentre, randomised, controlled clinical trial. Lancet Respir Med 2014;2:698-705.
- Struik FM, et al. Nocturnal non-invasive ventilation in COPD patients with prolonged hypercapnia after ventilatory support for acute respiratory failure: a randomised, controlled, parallel-group study. Thorax 2014;69:826-34.
- Vogelmeier DF, et al. Global strategy for diagnosis, management, and prevention of COPD. Am J Respir Crit Care Med 2017;195:557-82.
- Ergan B, Oczkowski S, Rochwerg B, et al. European Respiratory Society Guideline on Long-term Home Non-Invasive Ventilation for Management of Chronic Obstructive Pulmonary Disease. Eur Respir J 2019; in press (https://doi.org/10.1183/13993003.01003-2019).
- Nocturnal non-invasive positive pressure ventilation for COPD. Windisch W et al. Expert Rev Respir Med. 2015 Jun; 9(3):295-308.
- Dreher M, et al. Noninvasive ventilation in COPD: impact of inspiratory pressure levels on sleep quality. Chest 2011;140:939-45.