Better sleep starts with understanding sleep apnea
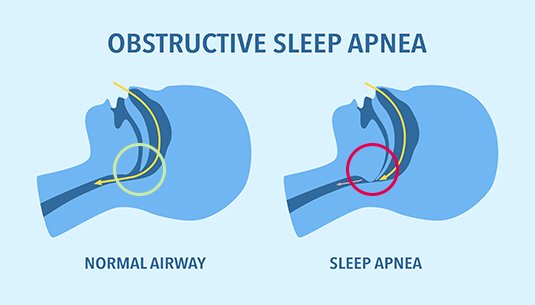
What exactly is sleep apnea?
Sometimes, breathing slows down or even stops for a few seconds or minutes. That’s sleep apnea, a sleep disorder where the throat muscles relax and block airflow.
As this cycle repeats throughout the night, it can deprive the body of the oxygen it needs to function at its best, day after day.
The real impact goes beyond just the physical. It can also affect us mentally and emotionally, leaving you constantly feeling like you’re running on a half-empty tank.
Roadmap to Rest:
Take the Sleep Assessment
Follow along on a journey of tackling exhaustion, getting diagnosed with sleep apnea, and finding relief through CPAP therapy.
4 simple steps to better sleep
Concerned about sleep apnea? Start here to learn how to sleep and breathe easier.

Step 1: Listen to your body and recognize signs of a sleep disorder
Recognizing the signs of sleep apnea, such as snoring, mood swings, headaches, and persistent daytime fatigue is an important step toward better sleep.
The disorder affects over 1 billion people worldwide,7 across all ages
and body types.
While that may sound alarming, you’re not alone, more than 80% of people with sleep apnea remain undiagnosed.8

Step 2: Start the conversation about sleep with your doctor
Start the conversation with your doctor about how you’ve been sleeping. They can assess your symptoms, review your medical history, and decide if a sleep test or referral to a specialist is needed.
A sleep test collects information from your body while you sleep, helping your doctor identify whether you have a sleep disorder.
You can also talk with a healthcare provider in person.
Download our Doctor’s Discussion Guide for more information
“Freedom to sleep well is life-changing.” – Stacy
Start your journey to better sleep
Find out if sleep apnea could be affecting your rest.
FAQs on sleep testing
Most insurance plans, including Medicare, may help pay for sleep tests, doctor visits and CPAP equipment if they are medically needed. You may have a copay for the doctor’s visit and part of the sleep test cost. Insurance often lowers the total price. Check with your provider to see what’s covered or click here to check your insurance now.
Waiting to receive the results of any test can feel unsettling—especially when it’s a test to diagnose a sleep disorder. There’s a waiting period that varies from person-to-person and can range from 2 days up to several weeks.
During a follow-up appointment, you’ll discuss the results of your sleep test with a doctor or sleep specialist. If diagnosed with sleep apnea, this is typically when you’ll find out your Apnea-Hypopnea Index (AHI), which determines the severity of the diagnosis.
If breathing stops for more than 10 seconds, this is known as an apnea. Apneas can occur dozens—even hundreds—of times per night without you noticing. When breathing slows down but doesn’t stop completely, this is considered a hypopnea. With a sleep test, doctors can use a scale called the Apnea-Hypopnea Index (AHI) to measure how many times per hour you either pause or stop breathing each night.22
The first step after any diagnosis is figuring out how best to treat it. And with sleep apnea, it’s important that treatment begins as soon as possible. The good news is that sleep apnea is well-understood, and effective treatments for sleep apnea are available.
Understanding your options for treatment can help you and your doctor make an informed decision about the steps you can take next.
Disclaimers:
The content on this website is for informational purposes only and is not intended as a substitute for professional medical advice, diagnosis or treatment.
Please note CPAP devices and sleep tests require prescription. Always refer to the device’s user guide for detailed and appropriate use instructions. Consult your healthcare professional/provider if you are concerned or have questions with your sleep health or treatment options.
References:
- Source: Wimms, A et al. Global prevalence of mild Obstructive Sleep Apnea in females. Sleep. 2023;46(Supplement_1)A234-A23
- Source: Gray EL, McKenzie DK, Eckert DJ. Obstructive Sleep Apnea without Obesity Is Common and Difficult to Treat: Evidence for a Distinct Pathophysiological Phenotype. J Clin Sleep Med. 2017 Jan 15;13(1):81-88. doi: 10.5664/jcsm.6394. PMID: 27655455; PMCID: PMC5181619.
- Source: Zasadzińska-Stempniak K, Zajączkiewicz H, Kukwa A. Prevalence of Obstructive Sleep Apnea in the Young Adult Population: A Systematic Review. J Clin Med. 2024 Feb 28;13(5):1386. doi: 10.3390/jcm13051386. PMID: 38592210; PMCID: PMC10931680.
- Source: Spicuzza L, Caruso D, Di Maria G. Obstructive sleep apnoea syndrome and its management. Therapeutic Advances in Chronic Disease. 2015;6(5):273-285. doi:10.1177/2040622315590318
- Source: Thompson et al. Sci Rep 12, 5127 (2022).
- Source: Young T, et al. Am J Respir Crit Care Med. 2003;167(9):1181.
- Source: Benjafield, A et al., (2025). The Lancet Resp Med. DOI: 10.1016/S2213-2600(25)00002-5.
- Source: Gurubhagavatula I, et al., (2023). Obstructive Sleep Apnea Indicator Report. American Academy of Sleep Medicine.
- Source: Kapur et al. J Clin Sleep Med. 2017 Mar 15;13(3):479-504.
- Source: Corliss, J., (2020). Harvard Health.
- Source: Lance CG. Positive airway pressure: Making an impact on sleep apnea. Cleve Clin J Med. 2019;86(9 Suppl 1):26-33. https://www.ccjm.org/content/86/9_suppl_1/26
- Source: Wilbanks J. Sleep apnea sleep disorder – sleep education by AASM. Sleep Education. January 28, 2021. Accessed June 27, 2025. https://sleepeducation.org/sleep-disorders/obstructive-sleep-apnea/
- Source: Dobrosielski DA, Papandreou C, Patil SP, Salas-Salvadó J. Diet and exercise in the management of obstructive sleep apnoea and cardiovascular disease risk. Eur Respir Rev. 2017;26(144):160110. https://pubmed.ncbi.nlm.nih.gov/28659501/
- Source: Srijithesh PR, Aghoram R, Goel A, Dhanya J. Positional therapy for obstructive sleep apnoea. Cochrane Database Syst Rev. 2019;5(11):CD010990. https://pmc.ncbi.nlm.nih.gov/articles/PMC6491901/
- Source: Vega ME, Diaz-Abad M, Jaffe F, et al. Use of positional therapy when incorporated into a diagnosis-treatment algorithm for obstructive sleep apnea. Sleep Sci. 2019;12(1):15-20. https://pmc.ncbi.nlm.nih.gov/articles/PMC6508942/
- Source: Oral appliances for sleep apnea. Cleveland Clinic. August 4, 2023. Accessed June 27, 2025. https://my.clevelandclinic.org/health/treatments/21129-oral-appliance-therapy-for-sleep-apnea
- Source: Dieltjens M, Vanderveken O. Oral appliances in obstructive sleep apnea. Healthcare (Basel). 2019;7(4):141. https://pmc.ncbi.nlm.nih.gov/articles/PMC6956298/
- Source: Dana N. Beyond ozempic: The GLP-1 boom. Mayo Clinic Press. March 19, 2025. Accessed June 27, 2025. https://mcpress.mayoclinic.org/living-well/beyond-ozempic-the-glp-1-boom/
- Source: Diet MC. Considering GLP-1 medications? What they are and why lifestyle change is key to sustained weight loss. Mayo Clinic Diet. August 22, 2023. Accessed June 27, 2025. https://diet.mayoclinic.org/us/blog/2023/considering-glp-1-medications-what-they-are-and-why-lifestyle-change-is-key-to-sustained-weight-loss/
- Source: Cé PDS, Melo MES, Machado AA, Ridge SE, Fleury Curado T. Review of Neurostimulation Therapies for Obstructive Sleep Apnea: Hypoglossal Nerve Stimulation and Beyond. J Clin Med. 2025 Aug 4;14(15):5494. doi: 10.3390/jcm14155494. PMID: 40807116; PMCID: PMC12347120.
- Source: Obstructive Sleep Apnea: Learn More – Treatment of Obstructive Sleep Apnea. Institute for Quality and Efficiency in Health Care (IQWiG); 2022.
- Source: Heinzer, R., et al., Prevalence of sleep-disordered breathing in the general population: the HypnoLaus study. Lancet Respir Med, 2015